This is the second in a series of BLG publications to assist Ontario health care providers and organizations to understand and develop governance options as they work toward Ontario Health Team implementation.
OHT Update 2 – August
(PDF, 829 KB)
The Ontario government is moving forward with the creation of Ontario Health Teams (OHTs): integrated care delivery systems comprised of persons, entities or groups that have the ability to deliver, in an integrated and co-ordinated manner, at least three of the following types of services: Hospital, Primary care, Mental health or addictions, Home care or community care, Long-term care home and Palliative care.
OHT partners will include a wide range of different for-profit and not-for-profit entities and organizations.
We believe successful integrations and collaborations occur when participating health providers have adopted similar governance best practices. Health care providers who wish to be OHT members have an opportunity to assess and improve their governance as OHTs are forming and ensure they have adopted best practices.
This publication summarizes governance best practices for prospective OHT partner boards. This guidance will be of interest to all not-for-profit health care providers and organizations in Ontario, whether or not they are designated in the first wave of OHT or are in the "In Discovery" or "In Development" phase. It can also be used to guide OHT partners in identifying governance best practices to be adopted for the OHT itself as a governance framework is created for the development and decision-making process of an OHT – whether a formal “board” is established for that process, it is memorialized in a document such as a memorandum of understanding, or it is adopted as non-binding framework.
In order for health care organizations to build the trust and relationships necessary to move forward with OHT development, it is important that they are on the same page and speak the same language when it comes to governance best practices.
Framework for Good Governance
Good governance fundamentally means that boards carry out their fiduciary responsibilities.
The fiduciary role requires the board to act to ensure the corporation that it governs succeeds in serving its object or purposes (i.e., fulfilling its mission), and sustains itself in order to continue serving those objects by maintaining its tangible and intangible assets and financial viability. In doing so, the corporation adheres to its core values and discharges its accountability responsibilities.
The quality of governance is a direct result of the quality of the board’s behavior. Effective board behaviour is crucial for good governance.
There are three essential conditions that are conducive to and supportive of effective board behaviour:
- Board quality – the quality of the people at the table and the impact of their collective skills on good governance.
- Board role – the areas in which the board will exercise a governance role and the approach the board takes to exercise its role (i.e., what the board does).
- Board structures and processes – the structure and processes used by the board to perform its governance role (i.e., how the board does its work).
Objective: Mission/Values and Accountabilities
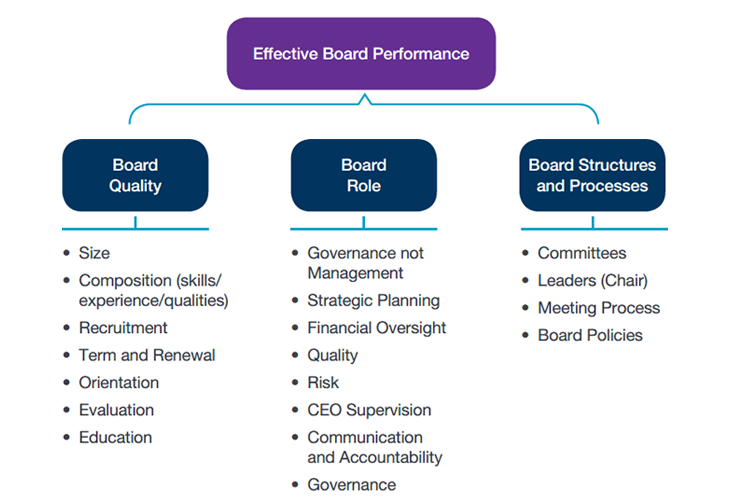
The best practices set out in this publication are fundamental in ensuring that a board has established the conditions for good governance. Best Practices #1, #2 and #3 relate to board quality. Best Practices #4, #5, #6 and #7 relate to the board's role. Best Practices #8, #9 and #10 address board structures and processes.
Board Quality
Best Practice 1: Board Recruitment
- Good governance starts with board quality. Board quality is a function of many factors including board size and composition. Board composition and recruitment processes will be impacted by the nature of the organization. Most OHT partners will have board recruitment processes that give the board the lead role in guiding board succession. When the board is accountable for board succession, the board should:
- recruit directors based on a skills/experience/diversity matrix that is annually reviewed and revised based on strategic directions,
- recruit directors with a view to future board leaders,
- use a variety of means to find board nominees,
- avoid situations of conflict by recruiting independent directors: ex officio directors are limited,
- ensure that renewal is not automatic and term limits are adhered to, and
- periodically review board size with reference to the work of the board.
Best Practice 2: Getting the Best from Each Director
- Once board quality is addressed, the board should ensure there are processes in place to enable each director to make a valuable contribution.
- The board (particularly the board chair) needs to takes ownership for the quality of director “on-boarding” (education, orientation, mentoring).
- The board needs to invest in ongoing governance education: at least one board meeting a year should include an education session on governance.
- Evaluations should be used to improve individual and collective performance and to make decisions about renewal.
- The chair should meet annually with each director and ask key questions, including soliciting feedback about the chair’s role and performance, but more importantly about the contribution to be expected of the director.
- Each director should be encouraged to have a personal development plan.
Best Practice 3: Director Engagement
- Individual directors must practice personal due diligence.
- Behaviour
- adhere to “rules” of fiduciary conduct,
- understand and respect the structures and processes of governance, and
- respect the chair and other directors.
- Participation
- fully engage in orientation and ongoing education, and
- recognize the importance of meetings – prepare, attend, participate.
- Commitment to Continuous Improvement
- personal development plan for contribution to the board over the course of board term.
Board Role
Best Practice 4: Shared Understanding of Board Role
- The board needs to have a shared understanding of the role of the board and the principles that apply to board decisions.
- The board must understand the importance of the board’s independent oversight of management and the need for the board to define “board work”.
- To better perform its role, the board should collectively spend time discussing the elements of acting in the best interests of the corporation particularly the corporation’s stakeholders and accountabilities: the board needs to understand its mission, vision, values and accountabilities, and to whom and for what the corporation is accountable.
- In health care, there are typically multiple and diverse stakeholders that need to be taken into account.
- The objective of corporate governance is to ensure the organization fulfils its mission, moves towards its vision, operates in a manner consistent with its values, and discharges its accountabilities.
- The board balances time spent in various responsibilities.
- The board adopts a written Board Role Statement to ensure the board has a shared understanding and to aid in board recruitment. A written Board Role Statement also assists the board in developing its Annual Board Work Plan, which in turn is an important tool in making meetings of the board effective.
Best Practice 5: Board Decision Process
- The board needs to understand the consensus decision process. The consensus decision process does not mean that a decision is unanimous but rather that all board members will support the decision even if they do not agree with it.
- A consensus decision process:
- is important for skills-based boards with multiple accountabilities, and
- ensures all sides of an issue are considered and allows a board with a diversity of skills and experience to ensure each director contributes their perspective to the discussion.
Best Practice 6: Boardroom Culture
-
The board and chair should establish and maintain processes to ensure that board culture enhances individual director and collective board contributions, and the risk of bad behaviour is minimized. Such processes will provide that:
- recruitment includes director behaviour,
- orientation includes expected behaviour, including attendance and adherence to the fiduciary standard,
- written Board Code of Conduct and Conflict of Interest polices are adopted but more importantly are understood by the board and enforced (peer influence),
- the board finds opportunities to build trust and collegiality, and
- the chair addresses behaviour issues in a timely manner.
Best Practice 7: Understand Health System Accountability and Adopt a System Perspective
The board needs a collective understanding of the accountabilities of the organization. Accountabilities of a publicly funded, mission-driven organization will be varied and include: patients/clients, other health care organizations, regulators, funders, donors, taxpayers, academic partners, the community served, etc. These varied accountabilities cause the board to have a health system perspective.
Looking at the organization through a system lens will impact key areas of the board role and function including:
- Strategic planning
- Recruiting – both at a board and management level
- Stakeholder relations and engagement
- Expectations of the board chair
Boards should:
- Be informed about health trends, the health system and, in particular, the local health system.
- Identify key stakeholder organizations and look for opportunities to build board-to-board relationships – such relationships can facilitate opportunities for integration by building trust and confidence.
- Evaluate decisions with reference to a system perspective. Where appropriate, boards should ask questions such as: “Have we talked to other key stakeholders in the system with respect to this initiative? How will this impact the system and other health care providers?”
- When the opportunity arises, participate in collaborative governance forums. If no such forums have been established, consider working with other health care providers to establish collaborative governance discussions facilitated by a neutral party.
Board Structures and Processes
Best Practice 8: Board Meetings are Effective
-
Board meetings are effective when the board understands and effectively uses the processes that enable effective board meetings. In health care organizations, these may be established or dictated by legislation and/or funding agreements. Such process includes:
- developing an Annual Board Work Plan to determine meeting frequency, specific agenda items and board education,
- structuring the board meeting agenda to ensure adequate time is allowed for discussion particularly for material board decisions and such decisions are not left to the end of the agenda,
- using a Consent Agenda to facilitate approval of routine or recurring matters where no debate is expected thereby allowing greater time for discussion of material matters,
- facilitating the board oversight function through the use of efficient performance oversight tools such as a balanced score card or dashboard,
- ensuring the board understands the role of committees and uses mechanisms to ensure efficient reporting from committees,
- using a decision support document for board decisions to ensure the board receives the information and analysis relevant for material decisions,
- ensuring the board collectively and the directors individually understand the fiduciary duties of directors and officers and behavioural expectations,
- the role of the chair as meeting manager is understood and respected by the board,
- adopting a written Code of Conduct for directors that addresses director behaviour generally, and in particular, issues of acceptable conduct during board meetings, and
if the board is required to have meetings that are open to the public, adopting a policy on in camera meetings.
- A board should ensure that it uses the meeting of independent directors without management present for the right reasons.
- A meeting of independent directors is not a board meeting: no decision binding on the corporation is to be taken during these sessions.
- Objectives are:
- ensuring board independence,
- allowing the board an opportunity to assess board process, particularly the adequacy and timeliness of information coming to the board from management,
- providing the opportunity to build relationships of confidence and cohesion among board members to improve board effectiveness, and
- ensuring the board is in a position to objectively evaluate performance of CEO and the board’s relationship with management—but this is not the CEO evaluation process.
-
Process:
- CEO remains for an initial period of time,
- CEO leaves, and
- Chair reports outcomes to CEO.
Best Practice 9: Board Committees are Effective
- It is important that the board understands why it has committees. In health care organizations, these may be established or dictated by legislation.
- committees are created by the board to assist with board work,
- committees (unless required by specific legislation) have no inherent right or role – all powers are derived from the board,
- committee terms of reference should be periodically reviewed, and
- the board must define board work first (Annual Work Plan helps).
Best Practice 10: The Chair is Effective
- The board and the chair need to have a shared understanding of the role of the chair. In particular:
- The chair is the board leader and ultimately accountable for the quality of board governance,
- The chair:
- ensures integrity and effectiveness of the board governance role and processes,
- is the presiding officer at board and member meetings,
- represents the board within the corporation and represents corporation/organization to community and/ or stakeholders, and
- builds relationships with board members, management and key stakeholders.
Additional Resources
The Guide to Good Governance: Not-for-Profit and Charitable Organizations (2013). Co-authored by Anne Corbett, Partner with BLG and Jim Mackay of Berkeley Consulting and published by the Ontario Hospital Association, offers governance tools, templates and guidance as a resource for developing and implementing the governance best practices referred to in this publication.
While the Ministry has provided guidance on minimum governance requirements for OHTs, it makes clear that governance arrangements for OHTs will be “self-determined and fit for purpose.” Good governance is key, not only for the operation of OHTs, but for individual providers, as a key ingredient in successful collaboration.
As providers and organizations come together at various stages in the OHT development process, they are looking for guidance with respect to OHT governance options, as well as solutions to provide structure and rigor to the development and decision-making required to form and operate OHTs.
BLG has released Governance Options: Getting Started and Evolving Towards Maturity (April 2019). This publication describes options for OHT governance.